There’s a virus you may never have encountered by name that is estimated to inhabit up to 90 percent of people and remains dormant in your cells for life—but if it becomes reactivated, it can devastate your brain. If that sounds alarming, researchers reported this week that there might be a newly identified trigger for activation—one that could affect as many as 10 percent of adults globally.
The agent is human polyomavirus 2, better known as the JC virus or John Cunningham virus, named after the patient from whom it was first isolated in 1971. It is detectable in the urine and stool of infected individuals and transmits via the fecal–oral route. Many people are believed to acquire it in childhood, and serologic surveys indicate that 50–90 percent of adults have encountered it at some point.
Investigators suspect the virus initially infects the tonsils or possibly the gastrointestinal tract. Wherever it enters, that first infection produces no symptoms. At that stage, a person carries what’s called the archetype JC virus, which establishes a persistent but clinically silent lifelong presence.
For most people, the JC virus remains harmless and asymptomatic. But in a small subset, the virus can awaken, rearrange its genome, and transform into a form that attacks the brain, causing a catastrophic disorder known as progressive multifocal leukoencephalopathy (PML).
Devastating disease
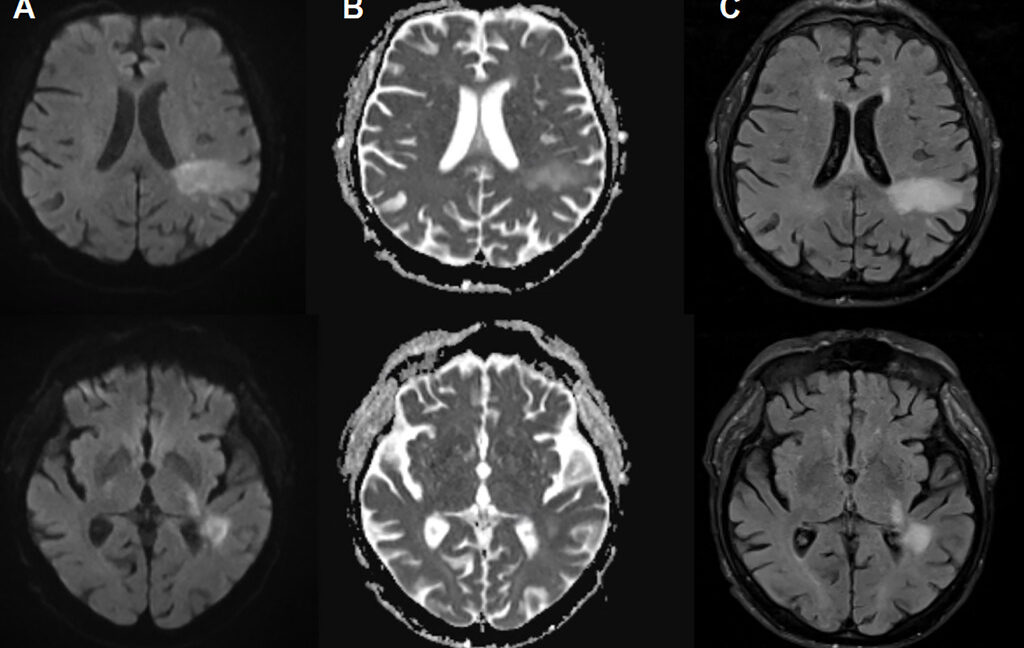
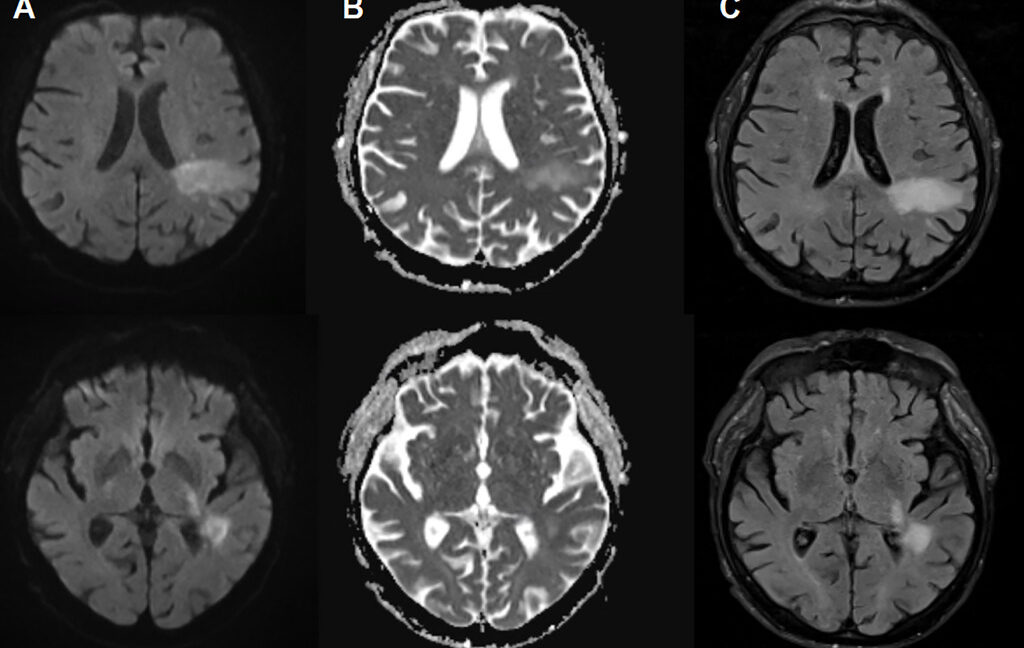
In PML, the mutated or “PML-type” JC virus invades the brain and destroys specific neural cells, including oligodendrocytes, which produce the myelin sheaths that insulate neurons. The result is widespread demyelination, leading to neuronal dysfunction and death. On scans, PML produces characteristic brain lesions; paired with detection of JC virus DNA in cerebrospinal fluid, these findings establish the diagnosis. Clinically, PML can mimic conditions from stroke to multiple sclerosis, producing symptoms such as speech problems, visual disturbances, motor deficits, and seizures.
PML was first described in 1958 in a cancer patient. It remained exceedingly rare until the 1980s, when cases began appearing in people with HIV/AIDS. Indeed, PML became an AIDS-defining illness, affecting 2–5 percent of HIV-infected patients early in the epidemic and at that time was uniformly fatal. After highly active antiretroviral therapy (HAART) was introduced in 1996, PML incidence fell and survival improved, though many survivors are left with substantial long-term impairment.